CHANGES OF THE SKIN [INTEGUMENTARY SYSTEM]
Alterations in hormonal balance and mechanical stretching are responsible for several changes in the integumentary system. The following changes occur during pregnancy:
- Linea Nigra; This is a dark line that runs from the umbilicus to the symphysis pubis and may extend as high as the sternum. It is a hormone-induced pigmentation. After delivery, the line begins to fade, though it may not ever completely disappear.
- Mask of Pregnancy (Chloasma); This is the brownish hyper pigmentation of the skin over the face and forehead. It gives a bronze look, especially in dark-complexioned women. It begins about the 16th week of pregnancy and gradually increases, and then it usually fades after delivery.
- Striae Gravidarum (Stretch Marks); This may be due to the action of the adrenocorticosteroids. It reflects a separation within underlying connective tissue of the skin. This occurs over areas of maximal stretch – the abdomen, thighs, and breasts. It will usually fade after delivery although they never completely disappear.
- Sweat Glands; Activity of the sweat glands throughout the body usually increases which causes the woman to perspire more profusely during pregnancy.
CHANGES OF BODY TEMPERATURE
- A slight increase in body temperature in early pregnancy is noted. The temperature returns to normal at about the 16th week of gestation.
- The patient may feel warmer or experience "hot flashes" caused by increased hormonal level and basal metabolic rate.
CHANGES OF THE BREASTS
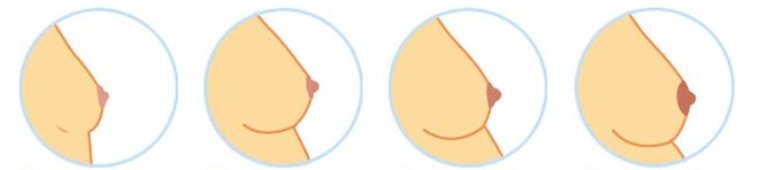 |
| Changes of the Breast during pregnancy - photo by The Alpha Parent |
- In early pregnancy, the breast may feel full or tingle, and increase in size as pregnancy progresses. The areolas of the nipples darken and the diameter increases. The Montgomery's glands (the sebaceous glands of the areola) enlarge and tend to protrude. The surface vessels of the breast may become visible due to increased circulation and turns to a bluish tint to the breasts.
- By the 16th week (2nd trimester) the breasts begin to produce colostrum. This is the precursor of breast milk. It is a thin, watery, yellowish secretion that thickens as pregnancy progresses. It is extremely high in protein.
- Nursing implication: Inform the pregnant patient to wear a good, supporting bra.
CHANGES IN BODY WEIGHT
- Normal weight gain is about 24 to 30 pounds (i.e. 10.9 to 13.6kg) during pregnancy.
- Weight gain in pregnancy;
- There is a slight loss of weight during early pregnancy if the patient experiences much nausea and vomiting.
- She then gains 2 to 4 pounds by the end of the first trimester.
- A gain of a pound per week is expected during the second and third trimesters.
- Monitoring of weight gain should be done in conjunction with close monitoring of blood pressure.
- A lack of significant weight gain may be an indication of intrauterine growth retardation (IUGR) of the infant.
- Patients with multiple fetuses will require a higher caloric diet and expect a higher weight gain than a patient with only one fetus.
- Adequate protein intake should be emphasized to the patient for development of the healthy fetus and proper diet reviewed at each prenatal visit.
CHANGES OF THE CIRCULATORY SYSTEM
Blood Volume.
- Blood volume increases gradually by 30 to 50 percent (1500 ml to 3 units). This results in decreased concentration of red blood cells and hemoglobin. This explains why the need for iron is so important during pregnancy.
- By the time pregnancy reaches term, the body has usually compensated for the decrease resulting in an essentially normal blood count.
- Blood count is interpreted as anemia by the physician if the hemoglobin falls below 10.5 grams per 100 ml and the hematocrit drops below 30 percent.
- Increased blood volume compensates for hypertrophied vascular system of enlarged uterus. It improves the placental performance. Blood lost during delivery; less than 500 cc (cubic centimeter, this is the same as ml) is normal (300 to 400 cc is average).
Cardiac Output.
- Cardiac output increases about 30 percent during the first and second trimester to accommodate for hypervolemia. This is not a problem for patients with a normal heart. A patient with a diseased heart is especially at risk for cardiac decomposition 28 to 35 weeks of pregnancy when the blood volume and cardiac load are at their peak; also, during labor and immediately after delivery when rapid hemodynamic changes occur.
- Change in output is reflected in the heart rate. It usually increases by 10 beats per minute.
- Nursing implication; Patients with a diseased heart need to be advised to get plenty of rest and to report any shortness of breath or unusual symptoms to their physician.
Blood Pressure.
- Normally, the patient's blood pressure will not rise.
- Nursing implications;
(a) The patient's blood pressure should be checked carefully and often since a significant increase is one of the indicators of toxemia (blood poisoning due to toxins) of pregnancy.
(b) When monitoring the blood pressure, be sure it is done under the same circumstances (that is, patient sitting and checking from the left arm).
- Venous Return.
- The lower extremities are often hampered in the last months of pregnancy due to the expanding uterus restricting physical movement and interfering with the return of blood flow. This results in swelling of the feet and legs.
- Nursing implications;
(a) Advise the patient to rest frequently. This will improve venous return and decrease edema.
(b) Have the patient to elevate her feet and legs while sitting.
(c) Remind the patient not to lie in a supine position since this inhibits return blood flow as the heavy uterus presses on the vessels. This leads to the vena cava syndrome or supine hypotension. The patient may complain of feeling dizzy, nauseated, or weak
CHANGES OF THE RESPIRATORY SYSTEM
- The respiratory rate rises to 18 to 20 cpm to compensate for increased maternal oxygen consumption, which is needed for demands of the uterus, the placenta, and the fetus.
- Women may feel out of breath and may need to sit a moment to catch their breath.
CHANGES OF THE URINARY SYSTEM
- The kidneys must work extra hard excreting the mother's own waste products plus those of the fetus. There is an increase in urinary output and a decrease in the specific gravity.
- The patient may develop urine stasis and pyelonephritis (inflammation of the kidney) in the right kidney. This is due to pressure on the right ureters resulting from displacement of the uterus slightly to the right by the sigmoid colon.
- Frequent urination is a complaint during the first through third trimester. As the uterus rises out of the pelvic cavity in early pregnancy, pressure on the bladder decreases and frequency diminishes. When lightening occurs during the final weeks of pregnancy, pressure on the bladder returns to cause frequent urination.
CHANGES OF THE SKELETAL SYSTEM
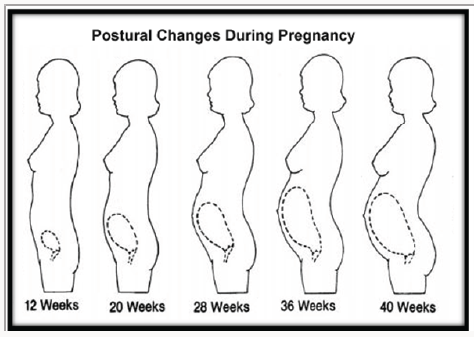
- There is a realignment of the spinal curvatures during pregnancy to maintain balance. It is due to the increase in size of the uterus and pressure on the abdominal wall. The patient walks with head and shoulders thrust backward and chest protruding outward to compensate. This gives the patient a "waddling" gait.
- There is a slight relaxation and increased mobility of the pelvic joints, which allows stretching at the time of delivery of the infant.
CHANGES OF THE GASTROINTESTINAL SYSTEM
- It was mentioned earlier that as the pregnancy progresses, the uterus enlarges. It rises up and out of the pelvic cavity. This action displaces the stomach, intestines, and other adjacent organs.
- Peristalsis is slowed because of the production of the progesterone, which decreases tone and mobility of smooth muscles. This slowing enhances the absorption of nutrients and slows the rate of secretion of hydrochloric acid and pepsin. Flare-up of peptic ulcers is uncommon in pregnancy. Slow emptying may increase nausea and heartburn (pyrosis). Relaxation of the cardiac sphincter may increase regurgitation and chance for heartburn. Movement through the large intestines is also slowed due to an increase in water consumption from this area. This increases the chance for constipation.
- Nursing implications.
(a) If the mother has difficulty with nausea and/or heartburn, advise her to eat small, frequent meals.
(b) The patient should eat a well-balanced diet high in protein, iron, and calcium for fetal growth; high fiber and fluids to prevent constipation.
(c) The mother should not lie flat for 1 to 2 hours after eating because this may cause heartburn and/or regurgitation.
CHANGES OF SELECTED GLANDS OF THE ENDOCRINE SYSTEM
- Parathyroid Gland; this gland increases in size slightly. It meets the increased requirements for calcium needed for fetal growth.
- Posterior Pituitary; Near the end of term, the posterior pituitary begins to secrete oxytocin that was produced in the hypothalamus and stored there. It will serve to initiate labor.
- Anterior Pituitary; At birth, the anterior pituitary begins to secrete prolactin. This stimulates the production of breast milk.
- Placenta. The placenta acts as a temporary endocrine gland during pregnancy. It produces large amounts of estrogen and progesterone by 10 to 12 weeks of pregnancy. It serves to maintain the growth of the uterus, helps to control uterine activity, and is responsible for many of the maternal changes in the body.







0 Comments