Introduction
It is the excessive discharge or escape of blood from broken blood vessels, caused by pathological condition of the vessels or by traumatic rupture of one or more vessels. In haemorrhage of any extent, there is also likely to be shock present and in this condition there is a lowered blood pressure.
Causes of haemorrhage
- Direct injury to the blood vessel wall.
- Disease of the blood vessel wall.
- Disease of the blood itself e.g. haemophilia.
Classification of Haemorrhage
Haemorrhage can be classified as follows
- According to the time it occurred – Primary, Reactionary and Secondary.
- According to the source – Vein, Artery, Capillary.
- According to the situation – Internal and External.
A. According to the time
Primary Haemorrhage
This occurs at the time of the injury or operation site or when the blood vessel has been damaged by disease.
Reactionary Haemorrhage
During haemorrhage, nature employs three agencies, to prevent serious loss of blood as follows;
- The blood pressure is lowered therefore there is diminished flow of blood to the part.
- A blood clot forms and 'corks' the blood vessel thus limiting further loss of blood.
- The blood-vessel walls 'turn in' to hold the clot in position and prevent further loss.
It is important to appreciate that up to twenty-four hours after an injury or operation, bleeding may commence once again. Reactionary haemorrhage occurs when the blood pressure, which was lower than normal, returns to normal and the clot is pushed out. This kind of haemorrhage can be recurring.
Secondary Haemorrhage
This type of haemorrhage seldom occurs, but if it does, it usually happens between seven and ten days after the injury or operation and is due to infection. When micro-organism infects a wound, they break down the clots.This usually takes several days to occur,thus secondary haemorrhage is slow to develop.lt is extremely dangerous and shows the importance of keeping wounds absolutely clean
B. According to the source
The following are indications that could suggest the source of bleeding;
Arterial bleeding
- Blood is bright red in colour due to oxygen-rich blood from the heart.
- Bleeding may be profuse.
- Blood will spurt out in time with heartbeat.
- If a main artery is damaged, it may jet blood several feet high. In this case the volume of circulating blood will fall rapidly.
Venous bleeding
- Blood from veins is dark red due to the presence of small amount of oxygen.
- It is under less pressure than arterial blood, but vein walls can widen greatly and the blood can "pool" inside it.
- If a major vein is damaged, blood may gush from it profusely.
Capillary bleeding
Bleeding from capillaries occurs with any wound especially superficial wounds.
- At first, bleeding may be brisk, but blood loss is usually slight.
- The colour of the blood may vary somewhat bright red to darker red.
- Blood generally oozes in small amounts.
C. According to the situation
Internal Haemorrhage; in these instance blood escapes from the vessel into a cavity or organ of the body or into the tissue. The simplest example of this type of haemorrhage is bruise or haematoma. It is possible for an internal haemorrhage to become visible, for example in bleeding of the alimentary tract, the person may eventually vomit up the blood.
Signs and Symptoms
Signs and symptoms of internal bleeding include;
- The pulse becomes weak rapidly.
- Skin becomes pale, cool and clammy.
- Air hunger or shortness of breath.
- The victim may faint or become dizzy.
- The victim may be thirsty, anxious and restless.
- The victim may be nauseated and may vomit.
External haemorrhage; this is the escape of blood from vessels through an open skin of the body to the external environment. Bleeding may stop on its own within minutes (6 on average) in minor wound, as the body uses its own defense mechanism to control bleeding.
General Sign and symptoms of Haemorrhage include;
- The skin becomes pale and cold.
- Subnormal temperature.
- The pulse is rapid and weak.
- Shortness of breath (air hunger).
- Anxiety and restlessness.
- Thirst.
- There may be obvious bleeding.
- Cyanosis may occur.
First Aid Management of Haemorrhage
Nature method
Nature immediately tries to stop excessive bleeding by performing three physiological tasks:
- By the formation of clot.
- The elastic coat of the blood vessel recoils and turns in; thus narrowing the lumen of the vessel and holding the clot.
- The blood pressure is lowered, thus there is less volume and pressure of blood in the vessels.
Internal Haemorrhage
It is important that any first-aid worker or nurse recognizes the signs and symptoms of internal haemorrhage although no bleeding can be seen, and waste no time in starting treatment.
- Perform primary assessment.
- The patient must be laid down, lying flat either on the floor, bed or crouch and kept absolutely still. If the patient is allow to move about in any way there is danger of further bleeding.
- Position the patient well, if possible the lower end of the bed or crouch can be raised. This may help the flow of blood by gravity to the brain and may prevent fainting or unconsciousness.
- Clothing around the neck, chest, and waits should not be tight. This will help patient to breath easily and prevent the feeling of suffocation.
- Assess the signs and symptoms and treat for shock if present.
- Reassure the patient.
- Arrange and transport patient to the hospital immediately.
External Haemorrhage
- Carry out primary assessment on the casualty.
- Make sure there are no foreign objects in the wound.
- Apply pressure directly to the wound.
- If the affected part is a limb, it should be raised as high as possible and maintained in position. This limits the flow of blood to the part and reduces the amount of the bleeding.
- Wash the affected part with clean water.
- Cover the wound as soon as possible with as clean as possible dressing and bandage it into a firm position.
- Direct pressure can be applied to artery known to supply the part. The pressure is applied to the artery where it passes the surface and superficially over the bone. These areas are Femoral artery, Radial artery, Brachial artery and Facial artery.
Direct pressure
Direct pressure is the main treatment used to manage severe bleeding:
- After checking for any foreign objects in the wound, apply firm pressure directly onto and into wound, using large sterile trauma dressings.
- If blood soaks through the initial dressing, apply further dressings as required
Application of Direct pressure
Emergency Tourniquet for arresting bleeding
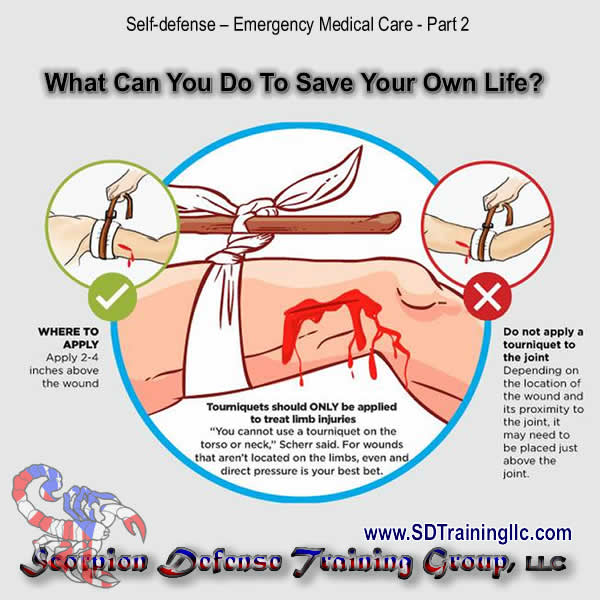 |
| Photo by Scorpion Defense Training Group, LLC |
- It must be tight enough.
- There must be a piece of material between the tourniquet and the skin.
- It must not left there for more than fifteen minutes (15min).
- An indication of the presence of a tourniquet must be made obvious.
Dangers associated with the use of tourniquet
- Likely to damage nerve and muscles.
- It is quite likely not to be tight enough therefore may not limit venous blood flow or stop arterial blood flow.
- If it is in the form of a narrow band it may easily damage the skin.
- There is serious danger if the tourniquet is left on for longer than twenty minutes (20mins).
How to use a tourniquet to arrest bleeding
To apply a tourniquet as a first aid measure, a tie, scarf or handkerchief can be used. This is applied round the upper arm or thigh, a knot tied, and a pencil or piece of stick used to tighten the band. This is done by placing the stick or pencil in the knot and rotating it, thus tightening the tourniquet.
Management of Special Haemorrhage
Epistaxis
Bleeding from the nose most commonly occurs when there is rupture of tiny, distended vessels in the mucous membrane of the nostrils.
There are a variety of causes associated with epistaxis, including trauma, infection, inhalation of illicit drugs, cardiovascular diseases, nasal tumors, low humidity, a foreign body in the nose, and a deviated nasal septum. Additionally, vigorous nose blowing and nose picking have been associated with epistaxis.
Management
- Put the casualty in sitting up position with the head tilt forward to allow the blood drain from the nostrils. This will prevent the swallow of blood.
- Loosen tight clothing and ask the victim to breathe through the mouth.
- Pinch the soft part of the nose firmly and advice victim to remain calm.
- Apply cold compress on the bridge of the nose and at the back of the neck.
- Transport victim if bleeding does not stop within 30 minutes.
- Once the bleeding has stopped, clean around the nose with lukewarm water.
- Advice the victim to rest quietly for few hours, avoid exertion so that blood clot is not disturbed.
Haemoptysis
This means coughing up blood. The blood coughed up is bright red in colour and frothy. The condition arises from any bleeding from the respiratory tract and the lungs.
Management
- Reassurance of victim to allay fear and anxiety.
- Place victim in a sitting position or propped up in bed.
- Loosen tight clothing.
- Ice may be given to victim to suck. This is helpful in upper respiratory bleeding.
- Keep stained specimen for inspection.
- Transport or call for doctor if severe.
Haematemesis
This is vomiting of blood. The bleeding may be coming from the upper GIT. Blood vomited is gritty and dark brown in colour and this is due to the fact that blood has been in contact with food and gastric secretions. This is sometimes referred to as 'Coffee ground sickness.
Management
- The patient should be immediately made to lie down.
- Tight cloths around the neck, chest and waist should be loosened.
- Reassurance is essential as the patient will be afraid, especially if vomiting is severe.
- The patient should be kept absolutely still and quiet. Any movement may increase the bleeding.
- The patient should not be given any thing by mouth, water may be given to rinse the mouth but should not be swallowed.
- Transport patient to hospital.
- All specimens of the vomit should be retained for the Doctor to inspect.
Haematuria
This term means blood in the urine. The blood may be escaping from the vessel in the kidneys, the ureters, the urethra, or the bladder. If small blood is lost, the urine will appear 'Smokey’ and if large amounts of blood are lost the urine will be bright red in colour. In extreme cases, very large amount of blood in the urine will make it appear very dark.
Management
- The patient should be made to rest comfortably in bed.
- Transport
the patient to the nearest health facility.Any
specimen of the urine should be kept for the Doctor to inspect.
Melaena
This describes blood in stool, when blood is lost from vessels high up in the intestinal tract, for example from a bleeding duodenal ulcer, it will make the stool appear black and tarry. The change in colour is due to the fact that intestinal juices have been in contact with the blood. Bright red blood may also be present in the stools, this occurs when there is damage near the lower end of the large intestines.
The term melaena means black, tarry stools.
Bleeding from the lower end of the intestinal tract may be due to:
- Heamorrhoids.
- Dysentery.
- Cancer of the lower bowel, particularly the rectum.
- Colitis.
Management
- The patient should be put to bed and kept quiet and still.
- All specimen of the stool or blood should be kept for inspection.
- Medical aid should be obtained as hospital treatment may be necessary.
Uterine Bleeding
Normally, blood escape from the uterus through the vagina at the menstrual period. Any bleeding occurring not associated with the menstrual period must be considered as a serious and urgent matter. Probably the commonest cause of uterine bleeding is a threatened abortion or miscarriage.
Management
- The patient must be put to bed immediately.
- The foot of the bed may be elevated, this can be done by placing a chair underneath the bottom of the bed.
- Reassure the patient and try to keep her absolutely still and quiet.
- Loosen tight clothing round the neck, chest, and waist.
- Apply a pad to the vulva and keep all pads for the doctor's inspection.
- Send for medical aid or transport the patient to the nearest health facility.






0 Comments