Introduction
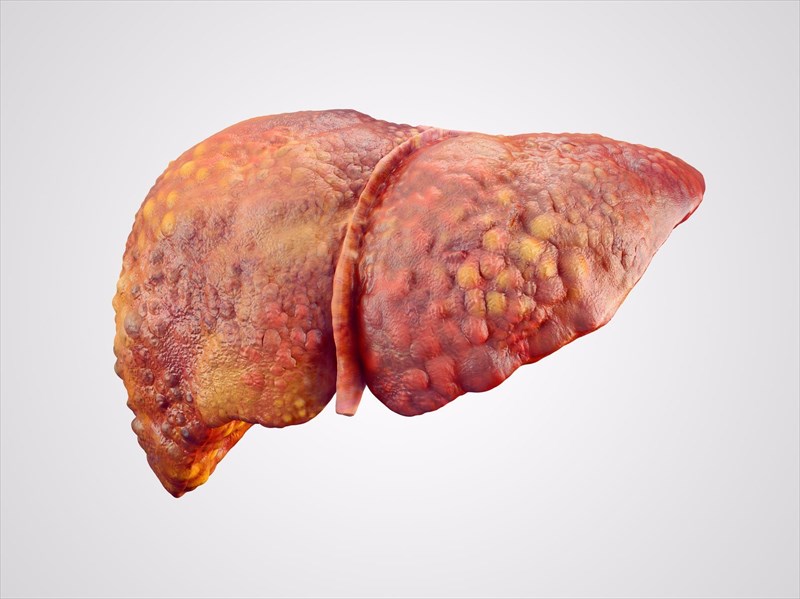
Cirrhosis is a progressive disease of the liver characterized by extensive degeneration and destruction of the liver parenchyma cells. When this happens, the liver cells attempts to regenerate but the regenerative process is disorganized resulting in abnormal blood vessel and diffuse fibrosis.
The fibrous connective tissue distorts the liver normal lobular structure. It may have an insidious and prolong course.
Causes
- Malnutrition
- Alcohol
- Infections e.g. hepatitis
The specific cause of cirrhosis may not be determined in all patients; it is known that cirrhosis occurs with greatest frequency among alcoholics. There have been cases of nutrition cirrhosis resulting from extreme dieting or malnutrition and it is believed that the combined impact of malnutrition and alcohol is damaging to hepatocytes. Alcohol alone has a direct hepatotoxic effect. It is known to cause necrosis of cell.
Types of Cirrhosis
- Alcohol cirrhosis
- Post necrotic cirrhosis: it is a complication of viral, toxic or idiopathic (autoimmune) hepatitis.
- Biliary cirrhosis: associated with chronic biliary obstruction and infection. There is diffuse fibrosis of the liver with jaundice as the main feature.
- Cardiac cirrhosis: results from prolong, severe right sided heart failure in patients with constrictive pericarditis.
Clinical Manifestation
- Onset usually proceeds in a gradual, subtle way but with harmful effects.
- Gastrointestinal tract disturbances are common early symptoms and include;
- anorexia
- nausea
- vomiting
- flatulence
- diarrhea or constipation
- The patient may complain of abdominal pain described as a dull heavy feeling in the right upper quadrant or epigastrium. The pain may be due to swelling and stretching of the liver capsule, spasm of the biliary ducts and intermittent vascular spasm.
- Fever
- Weight loss
- Distended abdomen.
- The liver is palpable in many patients with cirrhosis.
Diagnosis
- Physical examination
- Skin; jaundice
- Abdomen-tender hepatomegaly (palpable liver)
- Eyes; jaundice
- Laboratory investigations
- Serum bilirubin
- Prothrombin time
- Radiographic evaluation
- Ultrasonography to detect gallstone and dilation of common bile duct
- CT scan for detecting mass lesions in lever etc.
Treatment
- Generally, liver damage from cirrhosis cannot be reversed but treatment could stop or delay further progression and reduce complications.
- Alcoholic cirrhosis is treated by abstaining from alcohol.
- Medications that reduce itching may be given.
- Antibiotic may be given if there is infection. Neomycin sulphate is also give to decrease the formation of ammonia
- Massive hemorrhage requires blood transfusion.
- For portal hypertension, propranolol is a commonly used drug to lower blood pressure over the portal system etc.
Nursing Management
- Encourage bed rest.
- Observe for bleeding.
- Advice on skin care.
Complications
- Bleeding.
- Hepatic coma (hepatic encephalopathy); the liver cannot clear ammonia and related nitrogenous substances from the blood which are carried to the brain, affecting cerebral function.
- Intense itching.
Prognosis
Alcohol cirrhosis has a worst prognosis than primary biliary cirrhosis and cirrhosis due to hepatitis.
Read Also






0 Comments